Written by Frank Vickory SPT, CSCS
Parkinson’s Disease (PD) generally presents with some combination of four cardinal signs: Bradykinesia (slow movements), rigidity, resting tremor and postural instability. However, there are secondary symptoms of PD that can occur in many patients. One of the most common and potentially dangerous symptoms is Orthostatic Hypotension (OH). Fortunately, in the case of OH, a combination of medication, lifestyle modifications and hydration, patients can significantly reduce its harmful effects.
Definition and Pathophysiology of Orthostatic Hypotension
The American Academy of Neurology defines Orthostatic Hypotension as a drop in systolic blood pressure of 20mmHg or a drop in diastolic blood pressure of 10mmHg within three minutes of standing, when compared to a blood pressure in the sitting or supine position.1, 2 This large drop in blood pressure can result in the sensation of light-headedness, pallor of the face, weakness, fatigue, blurry vision or cognitive impairments. This often leads to a loss of balance when standing too quickly. And for patients with severe OH, they may even pass out, resulting in a fall.
Let’s not forget- falls are the leading cause of emergency department visits, hospitalizations and unintentional death in adults over the age of 65 years.3 This, coupled with the fact that PD patients are already at a higher risk for falling, puts people experiencing OH with PD at a very high risk for falls and injury.
Orthostatic Hypotension occurs from the blood dropping to your lower extremities with a change in position and the blood vessels in your lower extremities not responding fast enough to pump the blood throughout the body and most importantly the brain (cerebral perfusion). As a result, people with OH experience blood pooling in the lower extremity vessels, which limits blood supply back to the heart and brain (decreased cerebral perfusion).
Parkinson’s Disease and Orthostatic Hypotension
Research has suggested that patients with Parkinson’s Disease are at a higher likelihood for experiencing symptoms of Orthostatic Hypotension. Research has shown that between 31-40% of people with PD will have accompanying OH.4
When compared to national averages, OH is only prevalent in 5% of people under the age of 50. However, that number jumps to 30% of people over the ago of 70.5
These numbers suggest that older adults with PD are at a very high risk for experiencing OH. Because aging is directly correlated with increased occurrence of OH, the longer a patient lives with PD, the more likely they are to develop OH symptoms.
Treatment of Orthostatic Hypotension
From a treatment standpoint, there are many ways to manage symptoms and reduce the occurrence of OH. Conservative treatments include “warming up” prior to standing and being properly hydrated. If the symptoms cannot be alleviated with either of these conservative measures, medical treatment is an option in the form of medication.
Try This First:
Conservatively, preforming warm-ups prior to standing will help to get the blood pumping through the body. These pre-exercises can include ankle pumps, marching, kicks, etc. (See Image 1 for pictures). In fact, through virtually any movement, that will get your legs moving and help to promote blood pumping back into the rest of your body, will lessen the OH symptoms.
Try this Next:
Another conservative approach involves hydration. Continuous hydration throughout the day is vital for OH. The recommended water intake for adults is 64oz per day.
That is equivalent to the amount in a cranberry juice bottle: = 64oz
However, for patients that exercise regularly or have OH, the average water intake should actually be more than 64oz/day. Outside of continuous hydration, patients are encouraged to drink a whole glass of water (16oz) as fast as possible, prior to standing up, especially if they have been sitting for an extended period of time.6,7 The effects on blood pressure occur 5 minutes after drinking water and peak around 30 minutes after drinking the water. Meaning it is recommended to ingest the 16oz glass of water quickly, 5-30 minutes prior to standing. This includes standing after waking up in the morning or standing up after long bouts of watching TV or reading in the seated position.
If it’s still there…
From a medical standpoint, it is important to speak with your doctor prior to starting or stopping any medication. If you are experiencing similar symptoms to OH, talk to your doctor immediately. Especially, if you are on medications to lower your blood pressure, you may need to consult your primary care physician to see if there are any alterations that need to be made to your medication. If you are unable to make a same day appointment to speak with your primary care physician, ensure that you attempt the conservative treatments as to maintain safety from falling. The conservative treatments consist of the warm-up exercises and proper hydration.
Images:
Ankle Pumps: 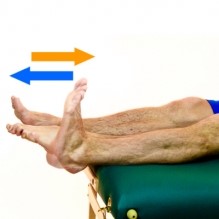 Knee extension:
Knee extension: 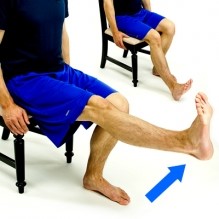 Hip Flexion:
Hip Flexion: 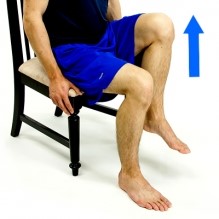
Key Points:
- Orthostatic Hypotension causes increased dizziness and falls. Parkinson’s Disease patients are already at a higher falls risk but are also far more susceptible to Orthostatic Hypotension.
- There are ways to combat Orthostatic Hypotension: Pre-standing “warm-ups” and proper hydration!! If problem persists, consult with physician about medication management.
References:
- Lanier JB, Mote MB, Clay EC (2011) Evaluation and management of orthostatic hypotension. Am Fam Physician 84: 527–536. pmid:21888303.
- Consensus statement on the definition of orthostatic hypotension, pure autonomic failure, and multiple system atrophy. The Consensus Committee of the American Autonomic Society and the American Academy of Neurology. Neurology. 1996;46(5):1470.
- Vincent GK, Velkoff VA. The Next Four Decades- The Older Population in the United States 2010to 2050:Population Estimates and Projections. August 2008.
- Velseboer DC, de Haan RJ, Wieling W, Goldstein DS, de Bie RM. Prevalence of orthostatic hypotension in Parkinson’s Disease: a systematic review and meta-analysis. Parkinsonism Relat Disord 2011;17:724–729.
- Ricci, F., De Caterina, R., & Fedorows, A. (2015). Orthostatic hypotension: Epidemiology, prognosis, and treatment. Journal of the American College of Cardiology, 66(7), 848-860.
- Jordan J, Shannon JR, Black BK, et al. The pressor response to water drinking in humans : A sympathetic reflex? Circulation. 2000 Feb 8; 101(5):504–9. [PubMed: 10662747]
- Jones, P. K., Shaw, B. H., & Raj, S. R. (2015). Orthostatic hypotension: managing a difficult problem. Expert review of cardiovascular therapy, 13(11), 1263.
